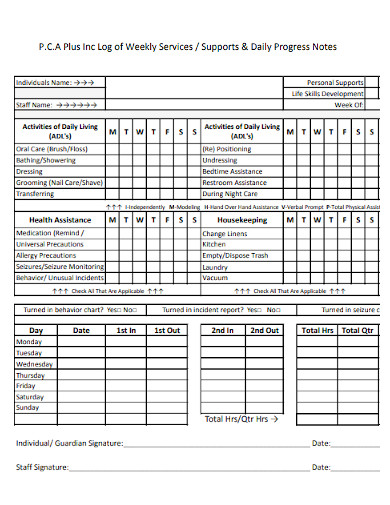
The consistent and accurate recording of patient progress is fundamental to effective healthcare. A well-structured Daily Progress Note Template provides a clear and concise record of a patient's condition, treatment response, and any relevant observations, facilitating seamless communication between healthcare providers and ensuring coordinated patient care. This template is designed to streamline the process, reducing errors and promoting proactive monitoring. Daily Progress Note Template is more than just a form; it's a tool for improving patient outcomes and optimizing clinical workflows. It's a critical component of patient-centered care, empowering clinicians to make informed decisions and address potential issues promptly. This detailed guide will walk you through creating and utilizing a robust Daily Progress Note Template, tailored to meet the diverse needs of various healthcare settings.
Understanding the Purpose of a Daily Progress Note
The primary purpose of a Daily Progress Note is to document a patient's condition and response to treatment daily. It's a snapshot of the patient's experience, providing a detailed account of their symptoms, interventions, and overall status. This information is invaluable for:
- Clinician Monitoring: Allows clinicians to quickly assess a patient's condition and identify any concerning trends.
- Treatment Adjustment: Enables adjustments to medication dosages, therapy plans, or other interventions based on observed changes.
- Communication: Facilitates clear and concise communication between healthcare providers, ensuring everyone is on the same page.
- Documentation & Compliance: Provides a readily available record for regulatory compliance and auditing purposes.
- Patient Empowerment: Offers patients a record of their care, promoting engagement and shared decision-making.
Key Components of a Comprehensive Daily Progress Note
A truly effective Daily Progress Note Template goes beyond simply recording data. It incorporates elements that promote thoroughness, accuracy, and clinical relevance. Here's a breakdown of the essential components:
- Patient Demographics: Include the patient's full name, date of birth, medical record number, and any relevant demographic information.
- Date and Time: Record the date and time the note was completed.
- Chief Complaint: A brief statement summarizing the patient's primary reason for seeking medical attention.
- Subjective Symptoms: Describe the patient's reported symptoms, including their severity, onset, and any associated factors (e.g., pain, nausea, fatigue).
- Objective Data: Document objective measurements, such as vital signs (temperature, blood pressure, heart rate, respiratory rate), lab results, and physical exam findings.
- Interventions: Detail any interventions performed, including medications administered, therapies provided, and any other actions taken.
- Response to Interventions: Assess the patient's response to each intervention. Did the intervention improve symptoms? Did it have any adverse effects?
- Assessment: Provide a concise assessment of the patient's condition, including their overall status and any areas of concern.
- Plan: Outline the next steps in the patient's care, including medication adjustments, follow-up appointments, and any further interventions.
Section 1: Detailed Assessment of Symptoms and Response to Treatment
This section is crucial for understanding the patient's current state and evaluating the effectiveness of treatment. It's a place to meticulously record observations related to the patient's symptoms and how they are responding to interventions.
- Symptom Severity: Rate the severity of each symptom using a standardized scale (e.g., 1-10, with 1 being mild and 10 being severe). Provide specific examples of how the symptom is impacting the patient's daily life.
- Associated Symptoms: Note any symptoms that are occurring concurrently with the primary complaint. These can provide valuable clues about the underlying cause of the patient's condition.
- Response to Medication: Document the patient's response to each medication administered. Is the medication effective in reducing symptoms? Are there any side effects that need to be addressed?
- Therapeutic Effectiveness: Assess the overall effectiveness of the treatment plan. Are the patient's symptoms improving? Are there any signs of worsening?
- Patient's Perspective: Include a brief statement from the patient regarding their experience with the symptoms and treatment. This can provide valuable insight into their subjective experience.
Daily Progress Note Template – Key Concept
This section is vital for tracking patient progress and identifying potential issues early on. It's not just about recording data; it's about understanding why the data is being recorded and how it relates to the patient's overall care. Regularly reviewing this section can highlight trends and potential problems before they escalate.
Section 2: Detailed Observations and Physical Examination Findings
This section provides a comprehensive record of the patient's physical examination findings. It's important to be specific and objective in your observations.
- Vital Signs: Record all vital signs, including temperature, blood pressure, heart rate, respiratory rate, and oxygen saturation. Note any significant deviations from the patient's baseline values.
- Skin Examination: Describe the patient's skin condition, noting any rashes, lesions, or other abnormalities.
- Head and Neck Examination: Document any findings related to the head and neck, such as swelling, tenderness, or bleeding.
- Respiratory Examination: Assess the patient's breathing patterns, noting any wheezing, shortness of breath, or chest wall movement.
- Neurological Examination: If applicable, document any neurological findings, such as weakness, numbness, or sensory changes.
- Musculoskeletal Examination: Describe any abnormalities in the patient's joints or muscles.
Daily Progress Note Template – Key Concept
The physical examination is a critical component of the patient's overall assessment. It provides objective data that can be used to confirm or refute subjective complaints. Always document findings in a clear and concise manner, using standardized terminology.
Section 3: Patient's Response to Lifestyle Modifications
This section addresses any changes in the patient's lifestyle that may be impacting their health.
- Dietary Habits: Document the patient's dietary intake, noting any changes in food preferences or restrictions.
- Exercise Routine: Record the patient's exercise routine, including the type, intensity, and duration of activity.
- Sleep Patterns: Document the patient's sleep patterns, noting any changes in sleep duration or quality.
- Smoking/Alcohol Use: Record the patient's smoking and alcohol use habits, and any attempts to quit or reduce their use.
- Social Support: Assess the patient's social support system, noting any factors that may be impacting their well-being.
Daily Progress Note Template – Key Concept
Lifestyle modifications are increasingly recognized as important components of patient care. Documenting these changes can help identify potential barriers to recovery and facilitate targeted interventions.
Section 4: Patient's Concerns and Preferences
This section allows for a space for the patient to express their concerns and preferences regarding their care.
- Expressing Concerns: Record any concerns the patient has about their condition or treatment.
- Patient Preferences: Document the patient's preferences regarding their care, including their desired treatment options and goals.
- Communication: Note any communication challenges the patient may be experiencing.
Daily Progress Note Template – Key Concept
Patient-centered care is paramount. Providing a space for the patient to voice their concerns and preferences is essential for fostering a collaborative and trusting relationship.
Conclusion
The Daily Progress Note Template is a powerful tool for improving patient care and optimizing clinical workflows. By consistently utilizing this template and tailoring it to the specific needs of each patient, healthcare providers can ensure that patients receive timely and effective care. Remember that the template is a guide, not a rigid set of rules. Flexibility and clinical judgment are essential for accurately and comprehensively documenting patient progress. Regular review and refinement of the template are also crucial for maintaining its effectiveness. Ultimately, the goal is to provide a clear, concise, and actionable record that supports informed decision-making and promotes positive patient outcomes. Daily Progress Note Template is a cornerstone of quality healthcare delivery.
0 Response to "Daily Progress Note Template"
Posting Komentar